10 ways South Africa can step up care for its healthcare workers
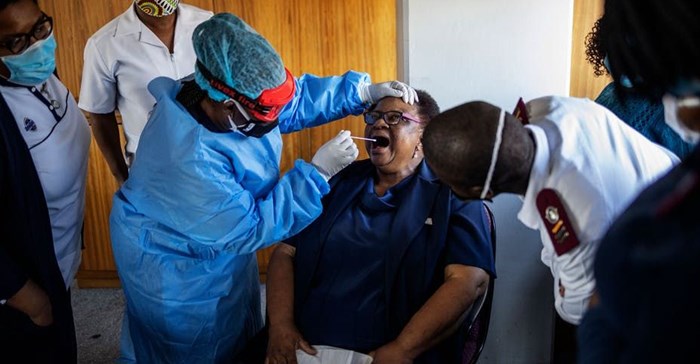
Covid-19 is rapidly adding to this problem. The International Council of Nurses estimates that about 230,000 – or 7% – of all Covid-19 cases worldwide are among healthcare workers.
In South Africa, healthcare workers have not been spared. By mid-July doctors, nurses, allied health workers, laboratory workers, paramedics or porters admitted to hospital accounted for 3% of total Covid-19 admissions.
The rates of infection and hospital admissions among healthcare workers is likely to increase as has been the case elsewhere in the world. The government recently allocated an additional R12.6bn (over $75m) to frontline health services.
But there’s no coherent welfare strategy for healthcare workers. There are medical protocols in place to reduce hospital and clinic staff’s risk of infection at work. But it’s not clear how the government seeks to assist staff with the extraordinary practical and psychological challenges of working daily – and over many months – with the threat of infection.
A welfare strategy should also include protocols for monitoring the effectiveness of plans and procedures to protect staff so that they can be revised if necessary. This will be inevitable as understanding of the virus improves.
Below we outline 10 elements of a coherent strategy to improve the welfare of healthcare workers as a result of Covid-19. These interventions are based on research and emergent practices in the field.
What a strategy should contain
Prioritise screening and testing for healthcare workers: The Imperial College London’s Covid-19 response team model shows that a regular testing approach on top of other measures, like healthcare workers self-isolating if they develop symptoms, could reduce staff’s contribution to transmission of the virus by 25%-33%. Some South African hospitals are using a dedicated staff tracker and report cases daily to the health department. In hospitals with limited testing kits, staff can conduct daily self-monitoring for Covid-19 symptoms.
There also needs to be vast improvement in the turnaround time (48 hours) for communicating test results. In public hospitals this can take as long as 12 days. It’s also recommended that in high Covid-19 prevalence areas, all incoming patients be treated as potential Covid-19 cases to improve infection control.
Provide adequate personal protective equipment and train people in how to use it: Health facilities still report not having enough quality personal protective equipment and it’s poorly used. Equitable distribution of personal protective equipment is also a concern. Provision of personal protective equipment has to be accompanied by frequent regular training and is an urgent priority.
Step up disinfection procedures: One hospital investigation showed the main way the virus spread was through droplets left on surfaces and transferred by health workers. Recent evidence on aerosol transmission of the coronavirus means that this vector of infection has been previously underestimated. Yet a recent report indicates that Covid-19 patients are being treated in same ward as non Covid patients.
Health facilities need support to reduce this means of transmission. This can be done by reviewing the ventilation, improving air filtration, installing ultraviolet lights, and disinfecting high-contact areas such as reception and communal eating spaces. Ensuring that Covid-19 patients are kept in isolation with minimal movement is important.
Step up mental health and support services: Healthcare workers are exposed to high levels of work stress. This can lead to mental exhaustion, anxiety and even post-traumatic stress disorders. Covid-19 also brings about issues of stigma because of the threat of infecting their families and others.
Professional and social support is required. There are some promising initiatives. For instance, a Cape Town based technology start-up, Vula Mobile, is being used nationwide to relieve distress through a mental health helpline for healthcare workers. A Healthcare Workers Care Network has been launched nationwide by the South African Society of Psychiatrists, the South African Medical Association, and the South Africa Depression and Anxiety Group to provide psychosocial support and education. But facilities need accessible on-site support.
Recruitment drive: South Africa currently has a shortage of more than 12,000 healthcare workers. More healthcare workers are likely to get sick or go into self-isolation. An urgent recruitment strategy is needed to increase personnel through volunteers, bursar nurses, intern and foreign doctors, and students. Staffing replenishment has to be paired with Covid-19 training to be effective.
Move to digital platforms: A new, ambitious digitisation project is being implemented at Tygerberg Hospital in the Western Cape to stop the spread of COVID-19 from patients to healthcare workers. The hospital is doing away with paper records in intensive care units while freeing up nursing capacity to focus on high-quality care to patients. More support is required for such innovations which can improve staff infection control by up to 50%.
Confront the risk and concerns: Healthcare workers are anxious about the possibility of infecting their families. As Covid-19 infections peak, more staff may wish to have alternative accommodation to avoid the risk of household transmission. The feasibility of using unoccupied student residences and hotels as temporary places for rest and self-isolation should be considered. Even the distribution of clear guidelines on how to reduce infection risks at home would help.
Provide financial motivation and dedicated transport: Given the ongoing salary disputes between healthcare workers and the government, incentives such as “risk allowances” could improve motivation. This was seen in the recent Ebola epidemic in West Africa. Dedicated transport to and from work can also limit risk of infections, as healthcare workers are not happy with public transport (for example, minivan taxis now allowed to function at full loading capacity).
Communicate between facility management and staff: There have been reports of some hospitals hiding information about positive cases in the workplace. Transparency and frequent communication is necessary to curtail infection. It could also address anxieties, curb fake news and reduce staff absenteeism. Using health and safety committees in hospitals to ensure Covid-19 compliance and communicate key health messages is important.
Provide financial compensation for illness or death: There should be coherent and free plans for the care of healthcare workers and their families.
As the Covid-19 epidemic intensifies, so too will the burden on healthcare workers. Healthcare workers are the country’s most important resource in the crisis response. In the face of these extraordinarily difficult challenges, the health ministry needs to be innovative and transparent in supporting healthcare workers.
This article is republished from The Conversation under a Creative Commons license. Read the original article.![]()
Source: The Conversation Africa

The Conversation Africa is an independent source of news and views from the academic and research community. Its aim is to promote better understanding of current affairs and complex issues, and allow for a better quality of public discourse and conversation.
Go to: https://theconversation.com/africa











