Top stories


Finance#AfricaMonth | Africa's next financial chapter will be driven by educated participation
Zihaad Israfil 25 May 2026



Often, parents and doctors aren’t immediately aware that there is a deformity or syndrome at play, and only after the baby displays breathing problems or other secondary ailments is there an investigation, which leads to a diagnosis.
Craniofacial surgery is designed to correct genetic conditions or deformations in the facial or skull areas. They can also be caused by trauma, tumours and complications from infections.
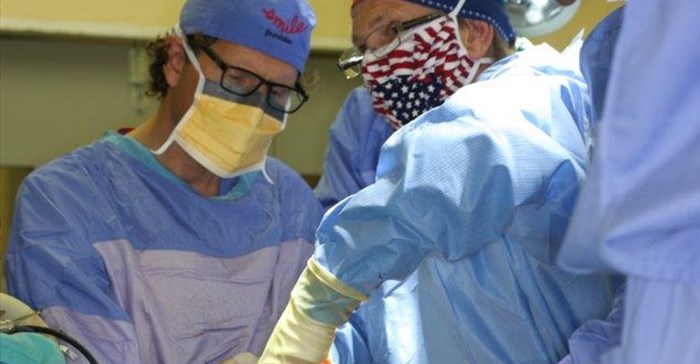
Often misunderstood to simply be facial or skull defects, it is important for parents (and their paediatricians) to know that craniofacial deformities are frequently more than just aesthetic. They can be accompanied by functional problems such as raised intracranial pressure, which sometimes leads to subtle developmental problems. The eyes can be affected by exophthalmos or amblyopia can develop.
Some patients have severe midface hypoplasia, a situation in which the upper jaw, cheekbones and eye sockets have not grown as much as the rest of the face. This can cause obstructive sleep apnoea and can eventually lead to heart failure.
We saw a case recently where a seven-year-old patient with severe midface hypoplasia suffered right-side cardiac failure due to increased pressure on the heart from breathing problems.
We performed a mid-face distraction and after one year post-op, the heart condition had clinically subsided, the patients breathing problems were significantly improved and there was a positive aesthetic outcome.
Medical science today has come a long way in diagnosing the various craniofacial deformities, and interventions have reached a very high standard in terms of surgical rectification at an early age to lessen the probability of complications arising.
It is understood that the majority of craniofacial syndromes are genetically caused, however, many of the individual genes causing these defects have not yet been identified. It is therefore not possible to treat before birth.
Those craniofacial syndromes that are apparent at birth display characteristics such as taller-than-usual head shape, a short head from front to back, tower-shaped, or long and narrow head from top to bottom (and so it continues). The head shape can be accompanied by poorly formed eye sockets, shallowly placed and protruding eyes, small eye openings and other eye defects along with a variety of other facial differences that can, in some syndrome cases, extend to serious and life-threatening defects such as heart defects, obesity, hearing, vision and breathing problems.
Those craniofacial deformities that are not as obvious at birth can become apparent in the first year of life as this is when the most rapid head growth occurs. An exception to this is Parry-Romberg syndrome, which usually starts in early adolescence (around 9 years of age). With this particular syndrome, the child may start noticing pigmentation changes to the skin, usually around the eye or cheek. Over time the tissue starts to wither away, leaving the child with severe facial asymmetry. The cause of this syndrome remains unknown.
In most craniofacial defect cases however, the skull bones of the baby’s head have not fused together at the right time, or in the right way. An exception is Goldenhar syndrome, where an embryonic blood vessel in the baby’s developing face may have accidently burst. But in all cases, it is important for parents to know that often the cause of the syndrome is genetic and in no way connected to anything that the mother could have prevented.
Congenital craniofacial defects which can be treated through surgery (which I’ll be discussing in this series) include:
All surgery treatments of craniofacial deformities and syndromes are done by a multidisciplinary team of specialists, in order to ensure the best outcome, the highest safety standards and the most efficient surgery.
In South Africa, there are only a few treatment centres with teams specialising and experienced in craniofacial surgery due to the rare incidence of craniofacial disorders. The multidisciplinary surgical team consists of a plastic surgeon specialised in craniofacial surgery, a paediatric neurosurgeon, an anaesthetists experienced with paediatric cases and sometimes a maxillofacial surgeon, especially if the lower jaw bones are involved.
Other related specialists that are an integral part of the planning process is the paediatrician, who is involved in diagnosing the condition and support in the peri-operative period, the geneticist to offer advice and support to parents and the treating team. Other related disciplines that might be necessary depending on the specific condition, include ophthalmologists and otolaryngologists, occupational therapists, physiotherapists and speech therapists.
In the article in the series, we’ll be discussing each syndrome and the various treatment options that are currently available to treat them. As well as outlining the developments and new techniques that employed in this field.