Where a person lives can drastically limit their access to trauma care. Around 5- billion people around the world lack reliable access to safe, affordable surgical and anaesthesia services, and most of these people live in low- and middle-income countries (LMICs), according to Dr Jim Yong Kim, former president of the World Bank.
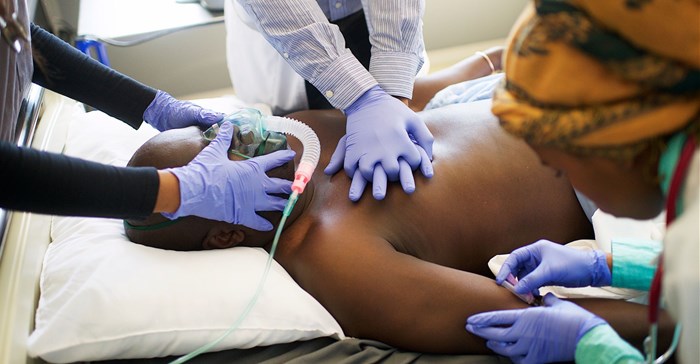
Image source: Getty/Gallo
Less than 6% of all surgeries are performed in the world’s poorest countries, even though these countries make up more than two-thirds of the world’s population. As a result, over 143-million surgical cases go untreated every year, almost 4.2-million of them in Central and sub-Saharan Africa.
Patients face many hurdles in accessing care, including delays in seeking, reaching and receiving care. The financial costs of seeking care can prevent underprivileged individuals from seeking care timeously.
Transportation
Ambulance transportation for the seriously ill or injured is a key element of access to trauma care, but remains unavailable to many. In South Africa, less than three quarters of seriously injured patients are transported by ambulance, according to the WHO. Additionally, a poor infrastructure and severe shortage of trained surgeons often means that facilities may not be appropriately equipped to handle these cases.
"Patients often need to be transported by an ambulance to different facilities. “Transporting patients under these conditions is very risky, and many patients will significantly deteriorate while being transported," says David Stanton, head of clinical Leadership at Netcare911 and speaker at the upcoming Africa Health Conference.
The lack of access to surgery, whether due to a shortage of anaesthetic drugs, transport or finances, means that every-day illnesses turn into life threatening emergencies, where people die from easily treatable conditions such as appendicitis, hernia, fractures and most worryingly, pregnancy and delivery.
Overcoming challenges
Awareness of the high number of easily preventable deaths due to limited access to this care is growing, and slowly giving rise to action. These efforts culminated in 2015 when the World Health Organisation's (WHO's) World Health Assembly passed a unanimous resolution calling for “strengthening emergency and essential surgical care and anaesthesia” as a central component of universal healthcare.
To support the WHO in their efforts, the Global Alliance for Surgical, Obstetric, Trauma, and Anaesthesia Care (G4 Alliance) was formed with the shared goal of "safe surgical and anaesthesia care for 80% of the world by 2030". For this ambitious target to be achieved, a number of intractable challenges must be overcome.
Finding solutions to these challenges is a slow process, but some progress is evident. For example, there are a few EMS systems working to upskill advanced life support (ALS) practitioners to reduce the number of adverse events that occur while transporting critically ill patients between health facilities. He warns that, “a concerted effort on the part of medical societies and practitioners will be required to ensure that those involved in transporting critically ill patients have the knowledge and skills to do so safely”.
Dearth of surgical skills
Kenya, a country of 5.8-million people, has only 18 anaesthetists and a dire shortage of anaesthetic and analgesic drugs”. Researchers are working to determine whether Ketamine could be used safely for emergency and essential procedures when no specialist is available.
The Lancet Commission for Global Surgery has established that meeting the need for surgery worldwide will require doubling the surgical workforce . In response, the College of Surgeons of East, Central and Southern Africa (Cosecsa) is working to train non-physician surgeons in countries with a limited number of doctors, to increase the surgical capacity in some of the most resource-poor areas of Africa. According to Dr Stephen Ogendo, past president of Cosecsa, many countries in sub-Saharan Africa already use non-physician surgeons to provide basic, low-cost essential surgeries. In Malawi, Mozambique and Tanzania, for example, about 90% of surgeries for maternity patients, including Caesarean sections, are performed by clinical officers.




















