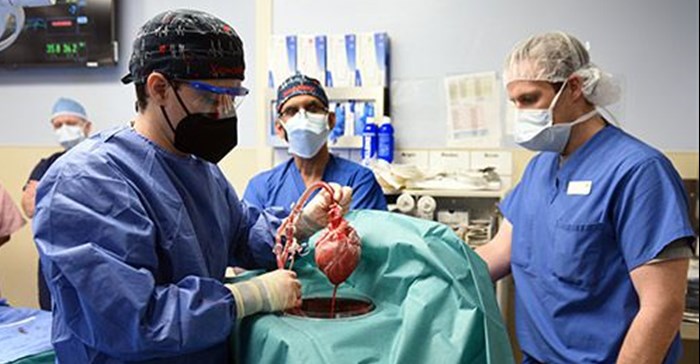
Man receives a genetically-modified pig heart in the world's first transplant of its kind
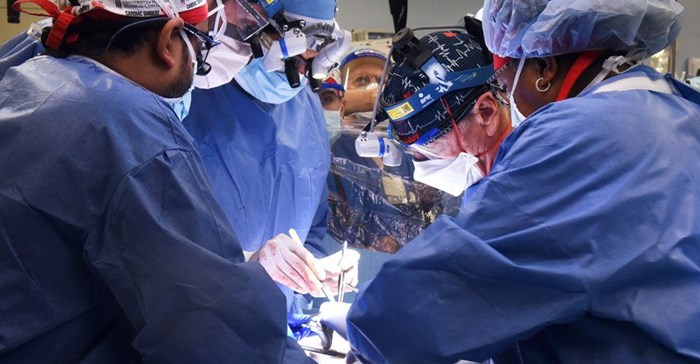
57-year-old David Bennett, who had a terminal heart disease, has received a genetically modified pig heart in a first-of-its-kind surgery in Maryland.
“It was either die or do this transplant. I want to live. I know it’s a shot in the dark, but it’s my last choice,” said Mr. Bennett, a day before the surgery was conducted. He had been hospitalised and bedridden for the past few months.
His son, David Bennett Jr. has confirmed that a week on, his dad is "very much alive and he’s talking to the nurses."
News of this first-of-its kind operation was hailed as a medical breakthrough.
“This is groundbreaking, this is remarkable and frankly, this is a miracle,'' said Bennett Jr. who said his dad was in the operating room three days straight. "He's got a lot of swelling throughout his body, but I know how strong my dad is. I know that his decision and desire to live, and his will, is greater than perhaps he even realises.''
Bennett Jr added that his dad had had some complications – like a collapsed lung at one point – but one of the nurses said he is doing better than some human-to-human heart transplant patients.
The team behind the record
A team at the University of Maryland School of Medicine (UMSOM) gave David Bennett Sr. the new heart.
After being diagnosed with terminal heart disease, the pig-to-human heart transplant was Bennett Senior’s last option.
Three genes previously linked with organ rejection were "knocked out" of the donor pig, and six human genes linked with immune acceptance were inserted.
This organ transplant demonstrated for the first time that a genetically-modified animal heart can function like a human heart without immediate rejection by the body.
The U.S. Food and Drug Administration granted emergency authorisation for the surgery on New Year’s Eve through its expanded access (compassionate use) provision. It is used when an experimental medical product, in this case the genetically-modified pig’s heart, is the only option available for a patient faced with a serious or life-threatening medical condition. The authorisation to proceed was granted in the hope of saving the patient’s life.
“This was a breakthrough surgery and brings us one step closer to solving the organ shortage crisis. There are simply not enough donor human hearts available to meet the long list of potential recipients,” said Bartley P. Griffith, MD, who surgically transplanted the pig heart into the patient.
“We are proceeding cautiously, but we are also optimistic that this first-in-the-world surgery will provide an important new option for patients in the future,” he said.
Years of research behind medical breakthrough
Considered one of the world’s foremost experts on transplanting animal organs, known as xenotransplantation, Muhammad M. Mohiuddin, MD, professor of surgery at UMSOM, joined the UMSOM faculty five years ago and established the Cardiac Xenotransplantation programme with Dr. Griffith. Dr. Mohiuddin serves as the programme’s scientific/programme director and Dr. Griffith as its clinical director.
“This is the culmination of years of highly complicated research to hone this technique in animals with survival times that have reached beyond nine months. The FDA used our data and data on the experimental pig to authorise the transplant in an end-stage heart disease patient who had no other treatment options,” said Dr. Mohiuddin. “The successful procedure provided valuable information to help the medical community improve this potentially life-saving method in future patients.”
If Bennett’s surgery proves successful, scientists hope pig organs could help alleviate shortages of human donor organs.
About 110,000 Americans are currently waiting for an organ transplant, and more than 6,000 patients die each year before getting one, according to organdonor.gov.